Neuroscientists get at the roots of pessimism
Stimulating the brain’s caudate nucleus generates a negative outlook that clouds decision-making.

Many patients with neuropsychiatric disorders such as anxiety or depression experience negative moods that lead them to focus on the possible downside of a given situation more than the potential benefit.
MIT neuroscientists have now pinpointed a brain region that can generate this type of pessimistic mood. In tests in animals, they showed that stimulating this region, known as the caudate nucleus, induced animals to make more negative decisions: They gave far more weight to the anticipated drawback of a situation than its benefit, compared to when the region was not stimulated. This pessimistic decision-making could continue through the day after the original stimulation.
The findings could help scientists better understand how some of the crippling effects of depression and anxiety arise, and guide them in developing new treatments.
“We feel we were seeing a proxy for anxiety, or depression, or some mix of the two,” says Ann Graybiel, an MIT Institute Professor, a member of MIT’s McGovern Institute for Brain Research, and the senior author of the study, which appears in the Aug. 9 issue of Neuron. “These psychiatric problems are still so very difficult to treat for many individuals suffering from them.”
The paper’s lead authors are McGovern Institute research affiliates Ken-ichi Amemori and Satoko Amemori, who perfected the tasks and have been studying emotion and how it is controlled by the brain. McGovern Institute researcher Daniel Gibson, an expert in data analysis, is also an author of the paper.
Emotional decisions
Graybiel’s laboratory has previously identified a neural circuit that underlies a specific kind of decision-making known as approach-avoidance conflict. These types of decisions, which require weighing options with both positive and negative elements, tend to provoke a great deal of anxiety. Her lab has also shown that chronic stress dramatically affects this kind of decision-making: More stress usually leads animals to choose high-risk, high-payoff options.
In the new study, the researchers wanted to see if they could reproduce an effect that is often seen in people with depression, anxiety, or obsessive-compulsive disorder. These patients tend to engage in ritualistic behaviors designed to combat negative thoughts, and to place more weight on the potential negative outcome of a given situation. This kind of negative thinking, the researchers suspected, could influence approach-avoidance decision-making.
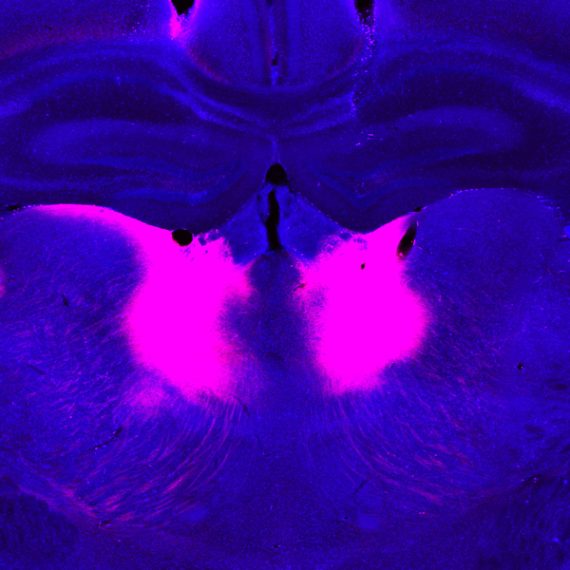
To test this hypothesis, the researchers stimulated the caudate nucleus, a brain region linked to emotional decision-making, with a small electrical current as animals were offered a reward (juice) paired with an unpleasant stimulus (a puff of air to the face). In each trial, the ratio of reward to aversive stimuli was different, and the animals could choose whether to accept or not.
This kind of decision-making requires cost-benefit analysis. If the reward is high enough to balance out the puff of air, the animals will choose to accept it, but when that ratio is too low, they reject it. When the researchers stimulated the caudate nucleus, the cost-benefit calculation became skewed, and the animals began to avoid combinations that they previously would have accepted. This continued even after the stimulation ended, and could also be seen the following day, after which point it gradually disappeared.
This result suggests that the animals began to devalue the reward that they previously wanted, and focused more on the cost of the aversive stimulus. “This state we’ve mimicked has an overestimation of cost relative to benefit,” Graybiel says.
The study provides valuable insight into the role of the basal ganglia (a region that includes the caudate nucleus) in this type of decision-making, says Scott Grafton, a professor of neuroscience at the University of California at Santa Barbara, who was not involved in the research.
“We know that the frontal cortex and the basal ganglia are involved, but the relative contributions of the basal ganglia have not been well understood,” Grafton says. “This is a nice paper because it puts some of the decision-making process in the basal ganglia as well.”
A delicate balance
The researchers also found that brainwave activity in the caudate nucleus was altered when decision-making patterns changed. This change, discovered by Amemori, is in the beta frequency and might serve as a biomarker to monitor whether animals or patients respond to drug treatment, Graybiel says.
Graybiel is now working with psychiatrists at McLean Hospital to study patients who suffer from depression and anxiety, to see if their brains show abnormal activity in the neocortex and caudate nucleus during approach-avoidance decision-making. Magnetic resonance imaging (MRI) studies have shown abnormal activity in two regions of the medial prefrontal cortex that connect with the caudate nucleus.
The caudate nucleus has within it regions that are connected with the limbic system, which regulates mood, and it sends input to motor areas of the brain as well as dopamine-producing regions. Graybiel and Amemori believe that the abnormal activity seen in the caudate nucleus in this study could be somehow disrupting dopamine activity.
“There must be many circuits involved,” she says. “But apparently we are so delicately balanced that just throwing the system off a little bit can rapidly change behavior.”
The research was funded by the National Institutes of Health, the CHDI Foundation, the U.S. Office of Naval Research, the U.S. Army Research Office, MEXT KAKENHI, the Simons Center for the Social Brain, the Naito Foundation, the Uehara Memorial Foundation, Robert Buxton, Amy Sommer, and Judy Goldberg.