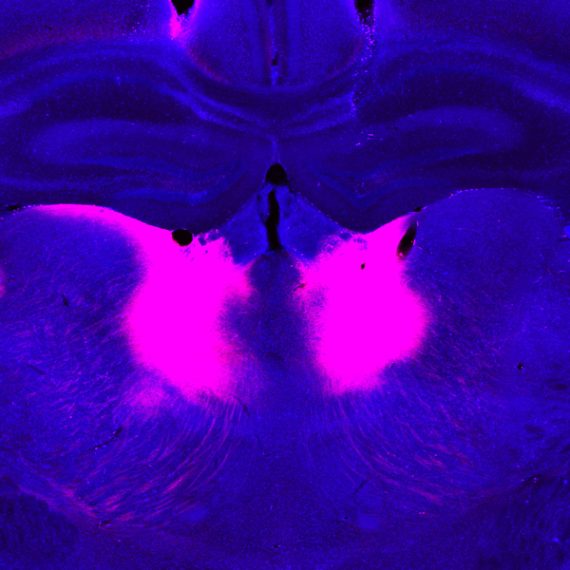
A new approach to curbing cocaine use
Activating a specific acetylcholine receptor in the brain reduces cocaine use in rodents.

Cocaine, opioids, and other drugs of abuse disrupt the brain’s reward system, often shifting users’ priorities to obtaining more drug above all else. For people battling addiction, this persistent craving is notoriously difficult to overcome—but new research from scientists at MIT’s McGovern Institute and collaborators points toward a therapeutic strategy that could help.
Researchers in MIT Institute Professor Ann Graybiel’s lab and collaborators at the University of Copenhagen and Vanderbilt University report in a January 25, 2022 online publication in the journal Addiction Biology that activating a signaling molecule in the brain known as muscarinic receptor 4 (M4) causes rodents to reduce cocaine self-administration and simultaneously choose a food treat over cocaine.
M4 receptors are found on the surface of neurons in the brain, where they alter signaling in response to the neurotransmitter acetylcholine. They are plentiful in the striatum, a brain region that Graybiel’s lab has shown is deeply involved in habit formation. They are of interest to addiction researchers because, along with a related receptor called M1, which is also abundant in the striatum, they often seem to act in opposition to the neurotransmitter dopamine.
Drugs of abuse stimulate the brain’s habit circuits by allowing dopamine to build up in the brain. With chronic use, that circuitry can become less sensitive to dopamine, so experiences that were once rewarding become less pleasurable and users are driven to seek higher doses of their drug. Attempts to directly block the dopamine system have not been found to be an effective way of treating addiction and can have unpleasant or dangerous side-effects, so researchers are seeking an alternative strategy to restore balance within the brain’s reward circuitry. “Another way to tweak that system is to activate these muscarinic receptors,” explains Jill Crittenden, a research scientist in the Graybiel lab.
New pathways to treatment
At the University of Copenhagen, neuroscientist Morgane Thomsen has found that activating the M1 receptor causes rodents to choose a food treat over cocaine. In the new work, she showed that a drug that selectively activates the M4 receptor has a similar effect.
When rats that have been trained to self-administer cocaine are given an M4-activating compound, they immediately reduce their drug use, actively choosing food instead. Thomsen found that this effect grew stronger over a seven-day course of treatment, with cocaine use declining day by day. When the M4-activating treatment was stopped, rats quickly resumed their prior cocaine-seeking behavior.
While Thomsen’s experiments have now shown that animals’ cocaine use can be reduced by activating either M1 or M4, it’s clear that the two muscarinic receptors don’t modulate cocaine use in the same way. M1 activation works on a different time scale, taking some time to kick in, but leaving some lasting effects even after the treatment has been discontinued.
Experiments with genetically modified mice developed in Graybiel’s lab confirm that the two receptors influence drug-seeking behavior via different molecular pathways. Previously, the team discovered that activating M1 has no effect on cocaine-seeking in mice that lack a signaling molecule called CalDAG-GEFI. M4 activation, however, reduces cocaine consumption regardless of whether CalDAG-GEFI is present. “The CalDAG-GEFI is completely essential for the M1 effect to happen, but doesn’t appear to play any role in the M4 effect,” Thomsen says. “So that really separates the pathways. In both the behavior and the neurobiology, it’s two different ways that we can modulate the cocaine effects.” The findings suggest that activating M4 could help people with substance abuse disorders overcome their addiction, and that such a strategy might be even more effective if combined with activation of the M1 receptor.
Graybiel’s lab first became interested in CalDAG-GEFI in the late 1990s, when they discovered that it was unusually abundant in the main compartment of the brain’s striatum. Their research revealed the protein to be important for controlling movement and even uncovered an essential role in blood clotting—but CalDAG-GEFI’s impacts on behavior remained elusive for a long time. Graybiel says it’s gratifying that this long-standing interest has now shed light on a potential therapeutic strategy for substance abuse disorder. Her lab will continue investigating the molecular pathways that underlie addiction as part of the McGovern Institute’s new addiction initiative.