Is it worth the risk?
McGovern researchers are studying how the brain balances risk and reward to make decisions.

During the Klondike Gold Rush, thousands of prospectors climbed Alaska’s dangerous Chilkoot Pass in search of riches. McGovern scientists are exploring how a once-overlooked part of the brain might be at the root of cost-benefit decisions like these. McGovern researchers are studying how the brain balances risk and reward to make decisions.
Is it worth speeding up on the highway to save a few minutes’ time? How about accepting a job that pays more, but requires longer hours in the office?
Scientists call these types of real-life situations cost-benefit conflicts. Choosing well is an essential survival ability—consider the animal that must decide when to expose itself to predation to gather more food.
Now, McGovern researchers are discovering that this fundamental capacity to make decisions may originate in the basal ganglia—a brain region once considered unimportant to the human
experience—and that circuits associated with this structure may play a critical role in determining our state of mind.
Anatomy of decision-making
A few years back, McGovern investigator Ann Graybiel noticed that in the brain imaging literature, a specific part of the cortex called the pregenual anterior cingulate cortex or pACC, was implicated in certain psychiatric disorders as well as tasks involving cost-benefit decisions. Thanks to her now classic neuroanatomical work defining the complex anatomy and function of the basal ganglia, Graybiel knew that the pACC projected back into the basal ganglia—including its largest cluster of neurons, the striatum.
The striatum sits beneath the cortex, with a mouse-like main body and curving tail. It seems to serve as a critical way-station, communicating with both the brain’s sensory and motor areas above, and the limbic system (linked to emotion and memory) below. Running through the striatum are striosomes, column-like neurochemical compartments. They wire down to a small, but important part of the brain called the substantia nigra, which houses the huge majority of the brain’s dopamine neurons—a key neurochemical heavily involved, much like the basal ganglia as a whole, in reward, learning, and movement. The pACC region related to mood control targeted these striosomes, setting up a communication line from the neocortex to the dopamine neurons.
Graybiel discovered these striosomes early in her career, and understood them to have distinct wiring from other compartments in the striatum, but picking out these small, hard-to-find striosomes posed a technological challenge—so it was exciting to have this intriguing link to the pACC and mood disorders.
Working with Ken-ichi Amemori, then a research scientist in her lab, she adapted a common human cost-benefit conflict test for macaque monkeys. The monkeys could elect to receive a food treat, but the treat would always be accompanied by an annoying puff of air to the eyes. Before they decided, a visual cue told them exactly how much treat they could get, and exactly how strong the air puff would be, so they could choose if the treat was worth it.
Normal monkeys varied their choices in a fairly rational manner, rejecting the treat whenever it seemed like the air puff was too strong, or the treat too small to be worth it—and this corresponded with activity in the pACC neurons. Interestingly, they found that some pACC neurons respond more when animals approach the combined offers, while other pACC neurons
fire more when the animals avoid the offers. “It is as though there are two opposing armies. And the one that wins, controls the state of the animal.” Moreover, when Graybiel’s team electrically stimulated these pACC neurons, the animals begin to avoid the offers, even offers that they normally would approach. “It is as though when the stimulation is on, they think the future is worse than it really is,” Graybiel says.
Intriguingly, this effect only worked in situations where the animal had to weigh the value of a cost against a benefit. It had no effect on a decision between two negatives or two positives, like two different sizes of treats. The anxiety drug diazepam also reversed the stimulatory effect, but again, only on cost-benefit choices. “This particular kind of mood-influenced cost-benefit
decision-making occurs not only under conflict conditions but in our regular day to day lives. For example: I know that if I eat too much chocolate, I might get fat, but I love it, I want it.”
Glass half empty
Over the next few years, Graybiel, with another research scientist in her lab, Alexander Friedman, unraveled the circuit behind the macaques’ choices. They adapted the test for rats and mice,
so that they could more easily combine the cellular and molecular technologies needed to study striosomes, such as optogenetics and mouse engineering.
They found that the cortex (specifically, the pre-limbic region of the prefrontal cortex in rodents) wires onto both striosomes and fast-acting interneurons that also target the striosomes. In a
healthy circuit, these interneurons keep the striosomes in check by firing off fast inhibitory signals, hitting the brakes before the striosome can get started. But if the researchers broke that corticalstriatal connection with optogenetics or chronic stress, the animals became reckless, going for the high-risk, high-reward arm of the maze like a gambler throwing caution to the wind. If they amplified this inhibitory interneuron activity, they saw the opposite effect. With these techniques, they could block the effects of prior chronic stress.
This summer, Graybiel and Amemori published another paper furthering the story and returning to macaques. It was still too difficult to hit striosomes, and the researchers could only stimulate the striatum more generally. However, they replicated the effects in past studies.
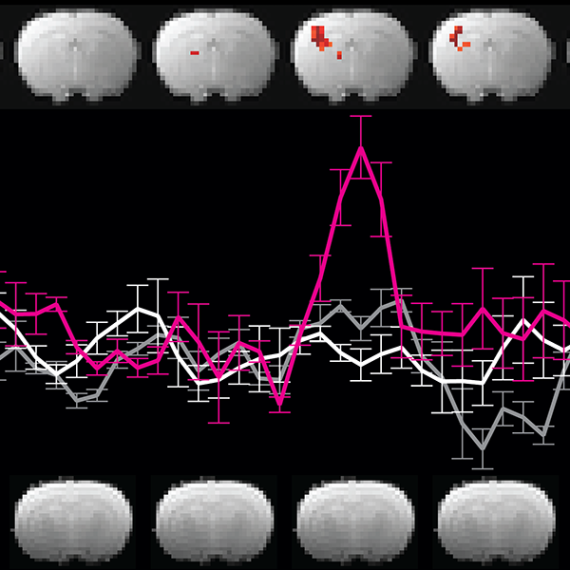
Many electrodes had no effect, a small number made the monkeys choose the reward more often. Nearly a quarter though made the monkeys more avoidant—and this effect correlated with a change in the macaques’ brainwaves in a manner reminiscent of patients with depression.
But the surprise came when the avoidant-producing stimulation was turned off, the effects lasted unexpectedly long, only returning to normal on the third day.
Graybiel was stunned. “This is very important, because changes in the brain can get set off and have a life of their own,” she says. “This is true for some individuals who have had a terrible experience, and then live with the aftermath, even to the point of suffering from post-traumatic stress disorder.”
She suspects that this persistent state may actually be a form of affect, or mood. “When we change this decision boundary, we’re changing the mood, such that the animal overestimates cost, relative to benefit,” she explains. “This might be like a proxy state for pessimistic decision-making experienced during anxiety and depression, but may also occur, in a milder form, in you and me.”
Graybiel theorizes that this may tie back into the dopamine neurons that the striosomes project to: if this avoidance behavior is akin to avoidance observed in rodents, then they are stimulating a circuit that ultimately projects to dopamine neurons of the substantia nigra. There, she believes, they could act to suppress these dopamine neurons, which in turn project to the rest of the brain, creating some sort of long-term change in their neural activity. Or, put more simply, stimulation of these circuits creates a depressive funk.
Bottom up
Three floors below the Graybiel lab, postdoc Will Menegas is in the early stages of his own work untangling the role of dopamine and the striatum in decision-making. He joined Guoping Feng’s lab this summer after exploring the understudied “tail of the striatum” at Harvard University.
While dopamine pathways influence many parts of the brain, examination of connections to the striatum have largely focused on the frontmost part of the striatum, associated with valuations.
But as Menegas showed while at Harvard, dopamine neurons that project to the rear of the striatum are different. Those neurons get their input from parts of the brain associated with general arousal and sensation—and instead of responding to rewards, they respond to novelty and intense stimuli, like air puffs and loud noises.
In a new study published in Nature Neuroscience, Menegas used a neurotoxin to disrupt the dopamine projection from the substantia nigra to the posterior striatum to see how this circuit influences behavior. Normal mice approach novel items cautiously and back away after sniffing at them, but the mice in Menegas’ study failed to back away. They stopped avoiding a port that gave an air puff to the face and they didn’t behave like normal mice when Menegas dropped a strange or new object—say, a lego—into their cage. Disrupting the nigral-posterior striatum
seemed to turn off their avoidance habit.
“These neurons reinforce avoidance the same way that canonical dopamine neurons reinforce approach,” Menegas explains. It’s a new role for dopamine, suggesting that there may be two different and distinct systems of reinforcement, led by the same neuromodulator in different parts of the striatum.
This research, and Graybiel’s discoveries on cost-benefit decision circuits, share clear parallels, though the precise links between the two phenomena are yet to be fully determined. Menegas plans to extend this line of research into social behavior and related disorders like autism in marmoset monkeys.
“Will wants to learn the methods that we use in our lab to work on marmosets,” Graybiel says. “I think that working together, this could become a wonderful story, because it would involve social interactions.”
“This a very new angle, and it could really change our views of how the reward system works,” Feng says. “And we have very little understanding of social circuits so far and especially in higher organisms, so I think this would be very exciting. Whatever we learn, it’s going to be new.”
Human choices
Based on their preexisting work, Graybiel’s and Menegas’ projects are well-developed—but they are far from the only McGovern-based explorations into ways this brain region taps into our behaviors. Maiya Geddes, a visiting scientist in John Gabrieli’s lab, has recently published a paper exploring the little-known ways that aging affects the dopamine-based nigral-striatum-hippocampus learning and memory systems.
In Rebecca Saxe’s lab, postdoc Livia Tomova just kicked off a new pilot project using brain imaging to uncover dopamine-striatal circuitry behind social craving in humans and the urge to rejoin peers. “Could there be a craving response similar to hunger?” Tomova wonders. “No one has looked yet at the neural mechanisms of this.”
Graybiel also hopes to translate her findings into humans, beginning with collaborations at the Pizzagalli lab at McLean Hospital in Belmont. They are using fMRI to study whether patients
with anxiety and depression show some of the same dysfunctions in the cortico-striatal circuitry that she discovered in her macaques.
If she’s right about tapping into mood states and affect, it would be an expanded role for the striatum—and one with significant potential therapeutic benefits. “Affect state” colors many psychological functions and disorders, from memory and perception, to depression, chronic stress, obsessive-compulsive disorder, and PTSD.
For a region of the brain once dismissed as inconsequential, McGovern researchers have shown the basal ganglia to influence not only our choices but our state of mind—suggesting that this “primitive” brain region may actually be at the heart of the human experience.